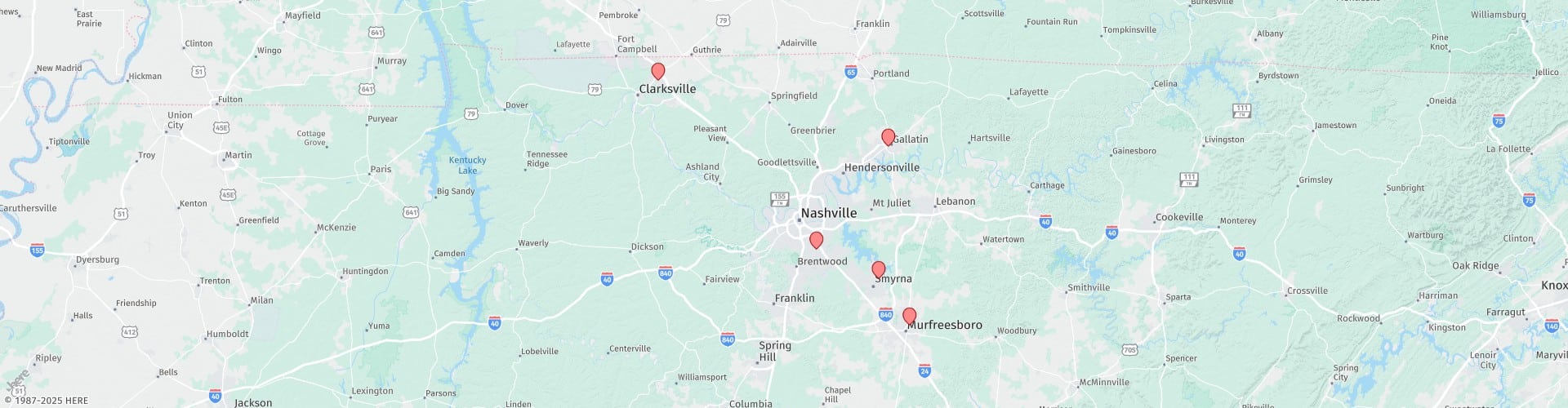
The esophagus is a muscular passageway for food and drinks that connects the oral cavity with the stomach. A muscular ring performs the sphincter closing function at the lower end of the esophagus, known as the lower esophageal sphincter (LES).
The sphincter prevents the reflux of food and gastric juice from the stomach to the esophagus. It opens as the bolus of food arrives at the lower end of the esophagus and allows the passage of food to the stomach.
Sometimes, irregularities arise in the closure of this sphincter that causes the reflux of acidic gastric juice back up into the esophagus. Oftentimes this causes a burning sensation called heartburn.
Random and infrequent episodes of acid reflux are typically not concerning. However, if reflux occurs frequently, it is known as Gastrointestinal Reflux Disease (GERD)(2). In this scenario, the acidic contents of the stomach gradually damage the outer lining of the esophagus, which can lead to a condition known as Barrett's esophagus.
Barrett's Esophagus
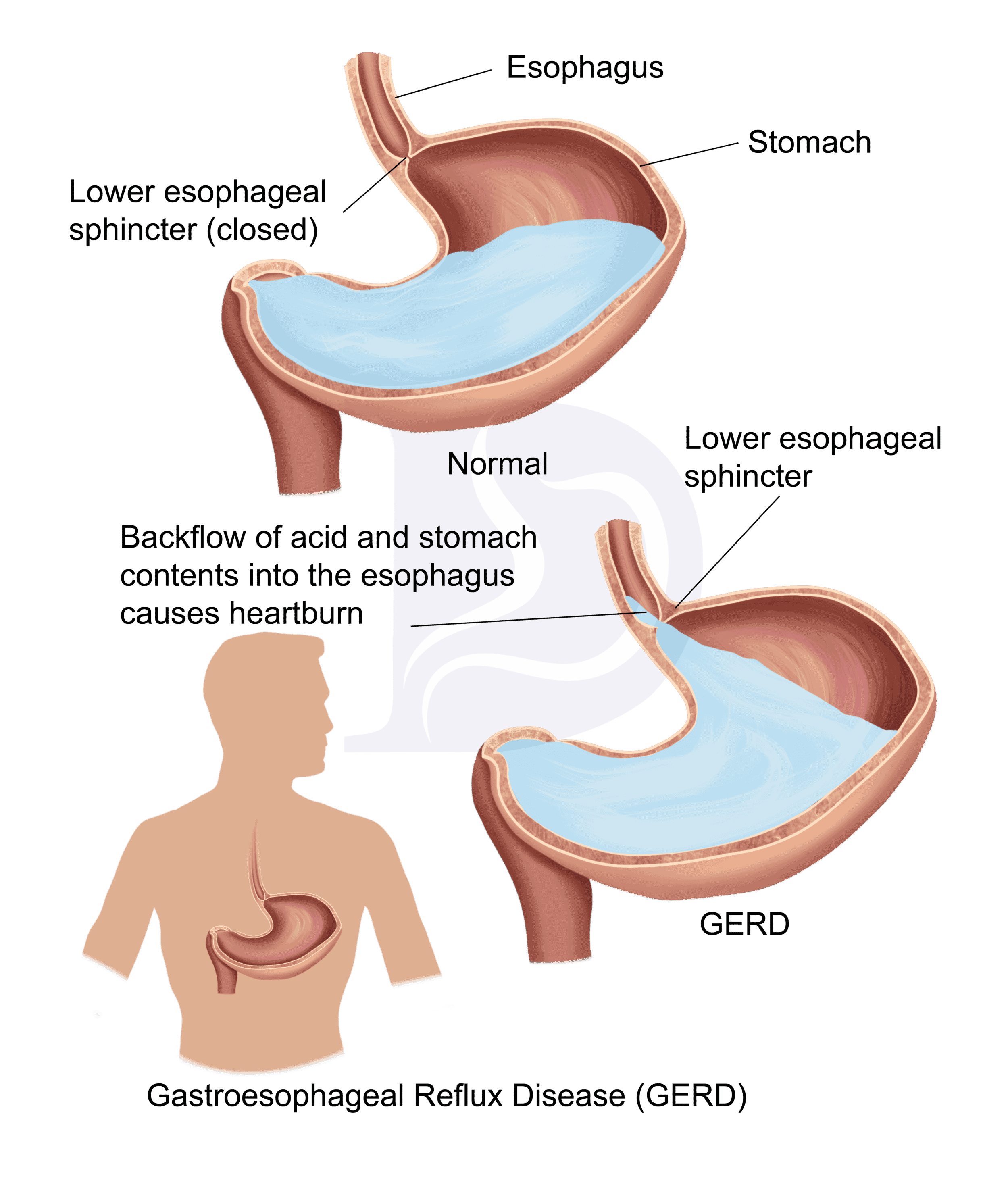
The epithelial lining of the esophagus is markedly different from the stomach and intestine. Both of these organs have adapted over centuries to their current functions. By examining the epithelial lining, it's easy to differentiate the tissue obtained from the esophagus or stomach.

The epithelium of the stomach has adapted to protect it from the harmful effects of stomach acid. The esophagus does not have the same adaptations. As a result, the lining of the esophagus can be severely damaged when constantly exposed to stomach acid. Due to continual exposure of the esophagus to acidic gastric contents, gastric epithelium eventually develops in the esophagus. This condition is called Barrett's esophagus.
As the epithelial lining of the esophagus changes, the symptoms of GERD alleviate, and the sensation of heartburn decreases in intensity.
However, the risk of cancer is greatly enhanced in the case of Barrett's esophagus(1). The more significant the epithelial transition, the greater is the risk of cancer.
Causes of Barrett's Esophagus
Barrett's esophagus is usually caused as a result of long-standing GERD. However, some people may have Barrett's esophagus without the warning signs of GERD. This condition is known as silent reflux.
Risk Factors of Barrett's Esophagus
Certain factors increase the risk of developing Barrett's esophagus, such as(3):
- Male gender
- Family history of Barrett’s
- Increasing age
- Overweight body habitus/Increased BMI
- Tea consumption
- Smoking and alcohol consumption (4)
Diagnosis
Barrett's esophagus is diagnosed during an endoscopy procedure. Surface abnormalities and the damage caused by acidic gastric contents are visualized during this procedure.
Biopsies of the lower esophagus near the esophageal sphincter are obtained if Barrett’s is suspected. In this process, a small tissue sample from the lower esophagus is excised and is examined under a microscope. These biopsies can confirm the disease (5).
Treatment
Several effective treatments are available now to treat Barrett's esophagus. As a result, the risk of developing cancer due to Barrett's esophagus has been significantly reduced for patients who seek early diagnosis and treatment.
Depending upon the severity of your condition, your provider will recommend medication or surgical treatment options.
Medication
The leading cause of Barrett's esophagus is acidic gastric contents. Certain medicines that decrease the stomach's acid production, such as omeprazole, lansoprazole, pantoprazole, etc., are used to treat gastric reflux(6).

Surgery
The lower esophageal sphincter can also be strengthened by surgery. It is done by minimally invasive procedures such as laparoscopy or fundoplication.
In these processes, the lower esophageal sphincter (LES) is tightened to prevent reflux into the esophagus. Barrett’s can also be treated in a procedure known as Radio Frequency Ablation (RFA), which essentially involves burning the “bad” tissues on the outer layer of the esophagus in order to promote growth a new healthy tissue. Your provider can discuss all these options in more detail during your office visits.
Prevention:
GERD and Barrett's esophagus can be prevented by:
- Adopting healthy eating habits.
- Avoidance of smoking and alcoholism.
- Avoidance of processed foods.
- Maintaining optimal body weight
The Bottom Line:
Barrett's esophagus is an adaptive response of the esophagus to chronic GERD that can progress to cancer if left untreated.
Fortunately, several treatments are available to manage chronic GERD and reduce the risk of Barrett's esophagus.
References
- Pixabay.com. Available from: https://pixabay.com/photos/heartburn-heartburn- symptoms-5273873/
- Richter JE, Rubenstein JH. Presentation and Epidemiology of Gastroesophageal Reflux Disease. Gastroenterology. 2018 Jan;154(2):267–76.
- Iyer PG, Kaul V. Barrett Esophagus. Mayo Clin Proc. 2019 Sep;94(9):1888–901.
- Chen Y-H, Yu H-C, Lin K-H, Lin H-S, Hsu P-I. Prevalence and risk factors for Barrett’s esophagus in Taiwan. World J Gastroenterol. 2019 Jul 7;25(25):3231–41.
- Shaheen NJ, Falk GW, Iyer PG, Gerson LB. ACG Clinical Guideline: Diagnosis and Management of Barrett’s Esophagus. Am J Gastroenterol. 2016 Jan;111(1):30–50; quiz 51.
- Hart AM. Evidence-based recommendations for GERD treatment. Nurse Pract. 2013 Aug 10;38(8):26–34; quiz 34–5.
- Pixabay.com. Available from: https://pixabay.com/photos/medicine-tablets-pills-health-2038745